Are Babies Attached to Mothers by the Umbilical Cord
| Umbilical cord | |
|---|---|
 Umbilical cord of a three-minute-old baby. A medical clamp has been applied. | |
| Details | |
| Identifiers | |
| Latin | funiculus umbilicalis |
| MeSH | D014470 |
| TE | cord_by_E6.0.2.2.0.0.1 E6.0.2.2.0.0.1 |
| Anatomical terminology [edit on Wikidata] | |
In placental mammals, the umbilical cord (also called the navel string,[1] nascency string or funiculus umbilicalis ) is a conduit between the developing embryo or fetus and the placenta. During prenatal development, the umbilical cord is physiologically and genetically part of the fetus and (in humans) commonly contains ii arteries (the umbilical arteries) and one vein (the umbilical vein), buried within Wharton's jelly. The umbilical vein supplies the fetus with oxygenated, nutrient-rich blood from the placenta. Conversely, the fetal eye pumps low oxygen, food-depleted blood through the umbilical arteries back to the placenta.
Structure and development [edit]

Cantankerous section of the umbilical string.

The umbilical cord develops from and contains remnants of the yolk sac and allantois. It forms by the fifth calendar week of development, replacing the yolk sac as the source of nutrients for the embryo.[2] The cord is non straight continued to the female parent'southward circulatory system, but instead joins the placenta, which transfers materials to and from the maternal blood without allowing directly mixing. The length of the umbilical cord is approximately equal to the crown-rump length of the fetus throughout pregnancy. The umbilical cord in a full term neonate is usually about fifty centimeters (xx in) long and about 2 centimeters (0.75 in) in diameter. This diameter decreases rapidly within the placenta. The fully patent umbilical artery has 2 main layers: an outer layer consisting of circularly arranged smooth muscle cells and an inner layer which shows rather irregularly and loosely arranged cells embedded in arable ground substance staining metachromatic.[3] The smooth musculus cells of the layer are rather poorly differentiated, comprise only a few tiny myofilaments and are thereby unlikely to contribute actively to the process of mail-natal closure.[3]
Umbilical cord can be detected on ultrasound by 6 weeks of gestation and well-visualised by 8 to 9 weeks of gestation.[iv]
The umbilical cord lining is a good source of mesenchymal and epithelial stem cells. Umbilical cord mesenchymal stem cells (UC-MSC) have been used clinically to treat osteoarthritis, autoimmune diseases, and multiple other conditions. Their advantages include a better harvesting, and multiplication, and immunosuppressive backdrop that ascertain their potential for use in transplantations. Their use would also overcome the ethical objections raised by the utilise of embryonic stem cells.[5]
The umbilical cord contains Wharton's jelly, a gelatinous substance made largely from mucopolysaccharides that protects the blood vessels inside. It contains one vein, which carries oxygenated, nutrient-rich claret to the fetus, and ii arteries that bear deoxygenated, nutrient-depleted blood away.[6] Occasionally, simply ii vessels (1 vein and i artery) are present in the umbilical string. This is sometimes related to fetal abnormalities, but information technology may likewise occur without accompanying issues.
It is unusual for a vein to carry oxygenated claret and for arteries to carry deoxygenated blood (the only other examples being the pulmonary veins and arteries, connecting the lungs to the heart). However, this naming convention reflects the fact that the umbilical vein carries claret towards the fetus'south center, while the umbilical arteries carry blood abroad.
The blood menstruum through the umbilical string is approximately 35 ml / min at 20 weeks, and 240 ml / min at forty weeks of gestation.[7] Adapted to the weight of the fetus, this corresponds to 115 ml / min / kg at 20 weeks and 64 ml / min / kg at xl weeks.[7]
For terms of location, the proximal part of an umbilical string refers to the segment closest to the embryo or fetus in embryology and fetal medicine, and closest to the placenta in placental pathology, and opposite for the distal part, respectively.[8]
Function [edit]
Connectedness to fetal circulatory system [edit]
The umbilical cord enters the fetus via the abdomen, at the bespeak which (later separation) will become the umbilicus (or bellybutton). Within the fetus, the umbilical vein continues towards the transverse fissure of the liver, where it splits into 2. One of these branches joins with the hepatic portal vein (connecting to its left branch), which carries blood into the liver. The second co-operative (known as the ductus venosus) bypasses the liver and flows into the inferior vena cava, which carries blood towards the heart. The 2 umbilical arteries co-operative from the internal iliac arteries and pass on either side of the urinary bladder into the umbilical cord, completing the circuit back to the placenta.[9]
Changes later birth [edit]
In absence of external interventions, the umbilical string occludes physiologically shortly afterwards nascence, explained both past a swelling and collapse of Wharton'south jelly in response to a reduction in temperature and by vasoconstriction of the blood vessels by smooth muscle wrinkle. In effect, a natural clench is created, halting the flow of claret. In air at 18 °C, this physiological clamping will take three minutes or less.[10] In h2o nascence, where the water temperature is close to body temperature, normal pulsation can be 5 minutes and longer.
Closure of the umbilical avenue by vasoconstriction consists of multiple constrictions which increment in number and degree with time. At that place are segments of dilatations with trapped uncoagulated blood between the constrictions before complete occlusion.[eleven] Both the partial constrictions and the ultimate closure are mainly produced by musculus cells of the outer circular layer.[iii] In contrast, the inner layer seems to serve mainly as a plastic tissue which can easily be shifted in an axial direction and so folded into the narrowing lumen to complete the closure.[three] The vasoconstrictive apoplexy appears to be mainly mediated by serotonin[12] [13] and thromboxane A2.[12] The artery in cords of preterm infants contracts more to angiotensin Ii and arachidonic acid and is more sensitive to oxytocin than in term ones.[thirteen] In contrast to the contribution of Wharton's jelly, cooling causes only temporary vasoconstriction.[13]
Within the kid, the umbilical vein and ductus venosus close up, and degenerate into fibrous remnants known equally the round ligament of the liver and the ligamentum venosum respectively. Part of each umbilical artery closes upward (degenerating into what are known every bit the medial umbilical ligaments), while the remaining sections are retained every bit role of the circulatory system.
Clinical significance [edit]
Issues and abnormalities [edit]

A knotted cord on a newborn baby
A number of abnormalities can affect the umbilical cord, which can crusade problems that affect both mother and child:[fourteen]
- Umbilical cord pinch can event from, for example, entanglement of the cord,[fifteen] a knot in the cord,[fifteen] or a nuchal cord,[15] (which is the wrapping of the umbilical cord around the fetal neck)[16] simply these conditions exercise not always crusade obstacle of fetal circulation.
- Velamentous cord insertion
- Single umbilical artery
- Umbilical cord prolapse
- Vasa praevia
Clamping and cut [edit]
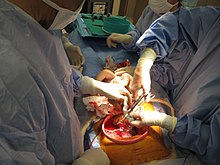
The umbilical string is almost to be cut with pair of scissors via cesarean department


A twenty-four hour period-onetime baby with its cord stump still attached.

A 7 cm (2.75 in) long discrete umbilical cord.
The string can be clamped at different times; however, delaying the clamping of the umbilical cord until at least one infinitesimal after nativity improves outcomes as long as there is the power to care for the minor risk of jaundice if it occurs.[17] Clamping is followed past cutting of the cord, which is painless due to the absence of fretfulness. The cord is extremely tough, similar thick sinew, and so cutting it requires a suitably sharp instrument. While umbilical severance may be delayed until later the string has stopped pulsing (i–three minutes after birth), there is ordinarily no significant loss of either venous or arterial claret while cutting the cord. Current evidence neither supports, nor refutes, delayed cutting of the cord, co-ordinate to the American Congress of Obstetricians and Gynecologists (ACOG) guidelines.
At that place are umbilical cord clamps which comprise a knife. These clamps are safer and faster, assuasive one to kickoff apply the cord clench and and then cut the umbilical string. After the cord is clamped and cut, the newborn wears a plastic prune on the navel expanse until the compressed region of the string has dried and sealed sufficiently.
The length of umbilical left fastened to the newborn varies by do; in most hospital settings the length of string left attached later clamping and cut is minimal. In the United States, however, where the birth occurred outside of the hospital and an emergency medical technician (EMT) clamps and cuts the cord, a longer segment upwards to 18 cm (7 in) in length[18] [nineteen] is left attached to the newborn.
The remaining umbilical stub remains for up to 10 days as it dries and then falls off.
Early versus delayed clamping [edit]
A Cochrane review in 2013 came to the determination that delayed cord clamping (between 1 and iii minutes after birth) is "probable to be beneficial as long as access to treatment for jaundice requiring phototherapy is available".[20] In this review delayed clamping, equally assorted to early, resulted in no difference in run a risk of astringent maternal postpartum hemorrhage or neonatal mortality, and a depression Apgar score. On the other hand, delayed clamping resulted in an increased birth weight of on average about 100 g, and an increased hemoglobin concentration of on boilerplate 1.v thousand/dL with half the risk of being atomic number 26 deficient at three and six months, but an increased hazard of jaundice requiring phototherapy.[20]
In 2012, the American College of Obstetricians and Gynecologists officially endorsed delaying clamping of the umbilical cord for xxx–threescore seconds with the newborn held beneath the level of the placenta in all cases of preterm delivery based largely on evidence that it reduces the chance of intraventricular hemorrhage in these children past 50%.[21] [ obsolete source ] In the same committee statement, ACOG likewise recognize several other likely benefits for preterm infants, including "improved transitional circulation, meliorate institution of crimson blood cell book, and decreased demand for blood transfusion". In January 2017, a revised Committee Opinion extended the recommendation to term infants, citing data that term infants benefit from increased hemoglobin levels in the newborn period and improved iron stores in the first months of life, which may result in improved developmental outcomes. ACOG recognized a small increase in the incidence of jaundice in term infants with delayed string clamping, and recommended policies exist in identify to monitor for and care for neonatal jaundice. ACOG likewise noted that delayed cord clamping is non associated with increased hazard of postpartum hemorrhage.[22]
Several studies have shown benefits of delayed string clamping: A meta-analysis[23] showed that delaying clamping of the umbilical cord in full-term neonates for a minimum of 2 minutes post-obit birth is beneficial to the newborn in giving improved hematocrit, iron status as measured by ferritin concentration and stored iron, as well as a reduction in the adventure of anemia (relative hazard, 0.53; 95% CI, 0.forty–0.70).[23] A decrease was also found in a study from 2008.[24] Although there is college hemoglobin level at 2 months, this effect did not persist across 6 months of historic period.[25] Not clamping the cord for three minutes following the nascency of a babe improved outcomes at four years of age.[26] A delay of three minutes or more in umbilical cord clamping afterwards nascence reduce the prevalence of anemia in infants.[27]
Negative effects of delayed string clamping include an increased adventure of polycythemia. Still, this condition appeared to be benign in studies.[23] Infants whose cord clamping occurred later than 60 seconds afterward birth had a higher rate of neonatal jaundice requiring phototherapy.[25]
Delayed clamping is not recommended as a response to cases where the newborn is non breathing well and needs resuscitation. Rather, the recommendation is instead to immediately clamp and cut the cord and perform cardiopulmonary resuscitation.[28] The umbilical cord pulsating is non a guarantee that the baby is receiving enough oxygen.[29]
Umbilical nonseverance [edit]
Some parents choose to omit cord severance entirely, a practice called "lotus nascence" or umbilical nonseverance. The entire intact umbilical cord is allowed to dry and separates on its ain (typically on the third day afterwards birth), falling off and leaving a healed umbilicus.[xxx]
Umbilical string catheterization [edit]
As the umbilical vein is straight connected to the key apportionment, it can be used as a route for placement of a venous catheter for infusion and medication. The umbilical vein catheter is a reliable culling to percutaneous peripheral or fundamental venous catheters or intraosseous canulas and may exist employed in resuscitation or intensive care of the newborn.
Claret sampling [edit]
From 24 to 34 weeks of gestation, when the fetus is typically viable, claret can be taken from the cord in order to test for abnormalities (particularly for hereditary conditions). This diagnostic genetic exam process is known as percutaneous umbilical string claret sampling.[31]
Storage of string blood [edit]
The claret inside the umbilical cord, known as cord blood, is a rich and readily bachelor source of primitive, undifferentiated stem cells (of type CD34-positive and CD38-negative). These string blood cells can be used for bone marrow transplant.
Some parents cull to have this blood diverted from the babe's umbilical blood transfer through early cord clamping and cutting, to freeze for long-term storage at a string blood banking company should the child ever crave the cord blood stem cells (for example, to supervene upon bone marrow destroyed when treating leukemia). This exercise is controversial, with critics asserting that early string blood withdrawal at the time of birth actually increases the likelihood of childhood illness, due to the high volume of blood taken (an average of 108ml) in relation to the baby's full supply (typically 300ml).[24] The Majestic College of Obstetricians and Gynaecologists stated in 2006 that "there is however insufficient evidence to recommend directed commercial string blood collection and stem-cell storage in depression-hazard families".[32]
The American University of Pediatrics has stated that cord blood cyberbanking for self-use should be discouraged (as virtually conditions requiring the use of stem cells volition already exist in the cord blood), while banking for general apply should exist encouraged.[33] In the future, cord claret-derived embryonic-like stem cells (CBEs) may exist banked and matched with other patients, much like blood and transplanted tissues. The use of CBEs could potentially eliminate the ethical difficulties associated with embryonic stem cells (ESCs).[34]
While the American Academy of Pediatrics discourages individual cyberbanking except in the instance of existing medical need, it also says that information about the potential benefits and limitations of cord blood banking and transplantation should be provided so that parents can brand an informed decision.
In the United States, cord blood educational activity has been supported by legislators at the federal and land levels. In 2005, the National University of Sciences published an Institute of Medicine (IoM) report which recommended that expectant parents be given a balanced perspective on their options for cord blood banking. In response to their constituents, state legislators across the country are introducing legislation intended to help inform physicians and expectant parents on the options for donating, discarding or banking lifesaving newborn stalk cells. Currently 17 states, representing 2-thirds of U.S. births, have enacted legislation recommended past the IoM guidelines.
The use of cord blood stem cells in treating atmospheric condition such as brain injury[35] and Type 1 Diabetes[36] is already beingness studied in humans, and earlier stage research is being conducted for treatments of stroke,[37] [38] and hearing loss.[39]
Cord blood stored with individual banks is typically reserved for utilise of the donor child only. In contrast, cord blood stored in public banks is accessible to anyone with a closely matching tissue type and demonstrated need.[40] The use of string blood from public banks is increasing. Currently it is used in place of a bone marrow transplant in the treatment of blood disorders such as leukemia, with donations released for transplant through ane registry, Netcord.org,[41] passing 1,000,000 as of Jan 2013. Cord blood is used when the patient cannot find a matching os marrow donor; this "extension" of the donor puddle has driven the expansion of public banks.
The umbilical cord in other animals [edit]
The umbilical string in some mammals, including cattle and sheep, contains two distinct umbilical veins. There is simply one umbilical vein in the man umbilical cord.[42]
In some animals, the mother will gnaw through the cord, thus separating the placenta from the offspring. The cord along with the placenta is frequently eaten by the mother, to provide nourishment and to dispose of tissues that would otherwise attract scavengers or predators.[ commendation needed ] In chimpanzees, the mother leaves the cord in place and nurses her immature with the cord and placenta attached until the string dries out and separates naturally, within a day of birth, at which time the cord is discarded. (This was starting time documented past zoologists in the wild in 1974.[43])
Some species of shark—hammerheads, requiems and smooth-hounds—are viviparous and have an umbilical cord fastened to their placenta.[44]
Animals that lay eggs seem to have a false umbilical-string that attaches the embryo and yolk together in much the same mode.[ citation needed ]
Other uses for the term "umbilical cord" [edit]
The term "umbilical cord" or but "umbilical" has also come to be used for other cords with similar functions, such as the hose connecting surface-supplied defined to their surface supply of air and/or heating, or space-suited astronauts to their spacecraft. Engineers sometimes use the term to describe a complex or disquisitional cable connecting a component, particularly when equanimous of bundles of conductors of dissimilar colors, thickness and types, terminating in a single multi-contact disconnect.
Cancer-causing toxicants in human umbilical cords [edit]
In multiple American and international studies, cancer-causing chemicals accept been establish in the blood of umbilical cords. These originate from sure plastics, computer excursion boards, fumes and synthetic fragrances among others. Over 300 chemical toxicants have been found, including bisphenol A (BPA), tetrabromobisphenol A (TBBPA), Teflon-related perfluorooctanoic acid, galaxolide and synthetic musks amidst others.[45] The studies in America showed higher levels in African Americans, Hispanic Americans and Asian Americans due, it is thought, to living in areas of higher pollution.[46]
Boosted images [edit]
-

Sectional plan of the gravid uterus in the third and quaternary month.
-

Fetus in utero, between fifth and sixth months.
-
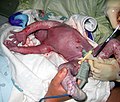
A newborn at 45 seconds, with umbilical cord clamped.
-
Umbilic. Deep dissection. Serial cantankerous section.
-

dried umbilical cord stump.
See also [edit]
- Belly button
- Umbilical line
References [edit]
- ^ "Umbilical – Search Online Etymology Dictionary". www.etymonline.com. Archived from the original on 4 March 2016. Retrieved 27 March 2018.
- ^ "The Umbilical Cord". yale.edu. Archived from the original on 28 March 2013. Retrieved 27 March 2018.
- ^ a b c d Meyer WW, Rumpelt HJ, Yao AC, Lind J (July 1978). "Construction and closure mechanism of the human being umbilical artery". Eur. J. Pediatr. 128 (4): 247–59. doi:10.1007/BF00445610. PMID 668732. S2CID 37516644.
- ^ Moshiri, Mariam; Zaidi, Sadaf F.; Robinson, Tracy J.; Bhargava, Puneet; Siebert, Joseph R.; Dubinsky, Theodore J.; Katz, Douglas S. (January 2014). "Comprehensive Imaging Review of Abnormalities of the Umbilical Cord". RadioGraphics. 34 (1): 179–196. doi:10.1148/rg.341125127. ISSN 0271-5333.
- ^ Saleh, R; Reza, HM (ten October 2017). "Short review on homo umbilical cord lining epithelial cells and their potential clinical applications". Stem Cell Research & Therapy. 8 (1): 222. doi:10.1186/s13287-017-0679-y. PMC5634865. PMID 29017529.
- ^ "Fetal Circulation". www.heart.org. Archived from the original on 22 December 2017. Retrieved 27 March 2018.
- ^ a b Kiserud, T.; Acharya, Grand. (2004). "The fetal circulation". Prenatal Diagnosis. 24 (13): 1049–1059. doi:10.1002/pd.1062. PMID 15614842. S2CID 25040285.
- ^ Mikael Häggström, MD (2020-08-27). Patholines https://patholines.org/Placenta.
- ^ "Peculiarities in the Vascular Organisation in the Fetus – Grey's Anatomy of the Human Body – Yahoo! Education". Archived from the original on January 23, 2012.
- ^ Cohain, J. Due south. (2010). "A Proposed Protocol for Third Stage Management – Judy'south 3,iv,5,10 minute method". Birth. 37 (1): 84–85. doi:10.1111/j.1523-536x.2009.00385_2.x. PMID 20402731.
- ^ Yao AC, Lind J, Lu T (1977). "Closure of the human being umbilical artery: a physiological demonstration of Burton'south theory". Eur. J. Obstet. Gynecol. Reprod. Biol. 7 (vi): 365–eight. doi:10.1016/0028-2243(77)90064-8. PMID 264063.
- ^ a b Quan A, Leung SW, Lao TT, Man RY (December 2003). "five-hydroxytryptamine and thromboxane A2 as physiologic mediators of human being umbilical artery closure". J. Soc. Gynecol. Investig. 10 (8): 490–5. doi:10.1016/S1071-5576(03)00149-7. PMID 14662162.
- ^ a b c White RP (Jan 1989). "Pharmacodynamic report of maturation and closure of human umbilical arteries". Am. J. Obstet. Gynecol. 160 (1): 229–37. doi:10.1016/0002-9378(89)90127-0. PMID 2912087.
- ^ "Umbilical Cord Complications: eMedicine Obstetrics and Gynecology". Archived from the original on 2010-01-29. Retrieved 2010-01-24 .
- ^ a b c P02.5 Fetus and newborn affected past other compression of umbilical string Archived 2014-11-02 at the Wayback Machine in ICD-10, the International Statistical Classification of Diseases
- ^ "Fetus or Newborn Problems: Labor and Delivery Complications: Merck Manual Abode Edition". Archived from the original on 2010-03-28. Retrieved 2010-03-27 .
- ^ McDonald, SJ; Middleton, P; Dowswell, T; Morris, PS (Jul 11, 2013). "Upshot of timing of umbilical cord clamping of term infants on maternal and neonatal outcomes". The Cochrane Database of Systematic Reviews. 7 (seven): CD004074. doi:10.1002/14651858.CD004074.pub3. PMC6544813. PMID 23843134.
- ^ Stiegler, Paul M., M.D. (May 2007). "EMT-BASIC \ EMT Bones INTERMEDIATE TECHNICIAN PROTOCOLS" (PDF). Dane Canton Emergency Medical Services. Archived (PDF) from the original on April half-dozen, 2012. Retrieved December 17, 2011.
{{cite spider web}}: CS1 maint: multiple names: authors list (link) - ^ Meersman, Jack. "EMT-B: Obstetrics, Infants and Children". Wild Iris Medical Educational activity. Archived from the original on January 20, 2012. Retrieved December 17, 2011.
- ^ a b McDonald, S. J.; Middleton, P.; Dowswell, T.; Morris, P. S. (2013). McDonald, Susan J (ed.). "Effect of timing of umbilical string clamping of term infants on maternal and neonatal outcomes". The Cochrane Database of Systematic Reviews. seven (seven): CD004074. doi:10.1002/14651858.CD004074.pub3. PMC6544813. PMID 23843134.
- ^ Commission on Obstetric Practice, American College of Obstetricians and, Gynecologists (December 2012). "Committee Stance No.543: Timing of umbilical string clamping later birth". Obstetrics and Gynecology. 120 (half-dozen): 1522–half-dozen. doi:10.1097/01.aog.0000423817.47165.48. PMID 23168790.
- ^ Committee on Obstetric Practice (2017-01-01). "Committee Opinion No. 684". Obstetrics & Gynecology. 129 (1): e5–e10. doi:ten.1097/aog.0000000000001860. ISSN 1873-233X. PMID 28002310.
- ^ a b c Hutton EK, Hassan ES (March 2007). "Late vs early clamping of the umbilical cord in full-term neonates: systematic review and meta-analysis of controlled trials". JAMA. 297 (eleven): 1241–52. doi:10.1001/jama.297.11.1241. PMID 17374818.
- ^ a b Test of the Newborn & Neonatal Wellness: A Multidimensional Arroyo, p. 116-117
- ^ a b "Effect of timing of umbilical cord clamping of term infants on maternal and neonatal outcomes." Cochrane Database Syst Rev. 2008; (2):CD004074
- ^ Andersson, O; Lindquist, B; Lindgren, Thou; Stjernqvist, K; Domellöf, M; Hellström-Westas, L (ane July 2015). "Result of Delayed String Clamping on Neurodevelopment at iv Years of Age: A Randomized Clinical Trial". JAMA Pediatrics. 169 (7): 631–viii. doi:10.1001/jamapediatrics.2015.0358. PMID 26010418.
- ^ "Can delayed umbilical cord clamping reduce infant anemia at age viii, 12 months?". medicalxpress.com. Archived from the original on 25 February 2018. Retrieved 27 March 2018.
- ^ Military Obstetrics & Gynecology – Delivery of the Baby Archived 2010-01-23 at the Wayback Machine The Brookside Assembly Medical Pedagogy Partitioning. Retrieved Jan 10, 2009
- ^ Waterbirth International – Waterbirth FAQ Retrieved Jan ten, 2009
- ^ Crowther, S (2006). "Lotus nascence: leaving the cord alone". The Practising Midwife. 9 (6): 12–fourteen. PMID 16830839.
- ^ "Man Reproduction, Lectures: Clinical Genetics". Retrieved 2010-02-11 .
- ^ "Umbilical Cord Blood Banking" (PDF) (Scientific Impact Newspaper eight). Royal College of Obstetricians and Gynaecologists. 2006. Retrieved 2021-07-01 .
{{cite web}}: CS1 maint: url-status (link) - ^ American University of Pediatrics. "Cord Blood Cyberbanking for Potential Future Transplantation". Archived from the original on 2007-10-13.
- ^ "Cord blood yields 'ethical' embryonic stem cells." Archived 2008-10-x at the Wayback Machine, Coghlin A. New Scientist, Baronial 18, 2005. Accessed June 25, 2007.
- ^ Cord Blood for Neonatal Hypoxic-Ischemic Encephalopathy Archived 2011-08-12 at Wikiwix, Autologous Cord Blood Cells for Hypoxic Ischemic Encephalopathy Study one. Stage I Study of Feasibility and Rubber
- ^ Haller MJ; Viener, HL; Wasserfall, C; Brusko, T; Atkinson, MA; Schatz, DA; et al. (2008). "Autologous Umbilical Cord Blood Infusion for Type 1 Diabetes". Exp. Hematol. 36 (6): 710–715. doi:10.1016/j.exphem.2008.01.009. PMC2444031. PMID 18358588.
- ^ Vendrame M, et al. (2006). "Cord blood rescues stroke-induced changes in splenocyte phenotype and function". Exp. Neurol. 199 (1): 191–200. doi:x.1016/j.expneurol.2006.03.017. PMID 16713598. S2CID 29804539.
- ^ Vendrame M, et al. (2005). "Anti-inflammatory effects of human being string claret cells in a rat model of stroke". Stalk Cells Dev. 14 (5): 595–604. doi:10.1089/scd.2005.14.595. PMID 16305344.
- ^ Revoltella RP, et al. (2008). "Cochlear repair by transplantation of human cord blood CD133+ cells to nod-scid mice made deafened with kanamycin and noise". Prison cell Transplant. 17 (6): 665–678. doi:x.3727/096368908786092685. PMID 18819255.
- ^ Najjar, Dana (2020-12-18). "Should Yous Banking company Your Baby's Cord Blood?". The New York Times. ISSN 0362-4331. Retrieved 2021-07-01 .
- ^ "Archived copy" (PDF). Archived (PDF) from the original on 2013-11-02. Retrieved 2013-04-13 .
{{cite spider web}}: CS1 maint: archived re-create every bit title (link) - ^ Meat Hygiene. J. F. Gracey, D. S. Collins, Robert J. Huey. p. 32.
- ^ See In the Shadow of Human, past Jane Goodall.
- ^ "Sharks (Chondrichthyes)". FAO. Archived from the original on 2008-08-02. Retrieved 2009-09-xiv .
- ^ Chen, Mei-Huei; Ha, Eun-Hee; Wen, Ting-Wen; Su, Yi-Ning; Lien, Guang-Wen; Chen, Chia-Yang; Chen, Pau-Chung; Hsieh, Wu-Shiun (3 Baronial 2012). "Perfluorinated Compounds in Umbilical Cord Claret and Adverse Birth Outcomes". PLOS ONE. 7 (8): e42474. Bibcode:2012PLoSO...742474C. doi:10.1371/journal.pone.0042474. PMC3411780. PMID 22879996.
- ^ "Why Are Trace Chemicals Showing up in Umbilical Cord Blood?". Scientific American. Archived from the original on 2012-09-02. Retrieved 2012-09-01 .
- Marianne Messerli; et al. (December 2013). "Stem Cells from Umbilical Cord Wharton'due south Jelly from Preterm Nativity Take Neuroglial Differentiation Potential". Reproductive Sciences. xx (12): 1455–1464. doi:ten.1177/1933719113488443. PMC3817666. PMID 23670950.
External links [edit]
-
 Media related to Umbilical cord at Wikimedia Commons
Media related to Umbilical cord at Wikimedia Commons
Source: https://en.wikipedia.org/wiki/Umbilical_cord

0 Response to "Are Babies Attached to Mothers by the Umbilical Cord"
Post a Comment